Health-care workers treating coronavirus need protective gear. In Pa. and N.J. they don’t have enough.
Medical personnel are resorting to creative — and potentially unsafe — tactics in the face of equipment shortages.
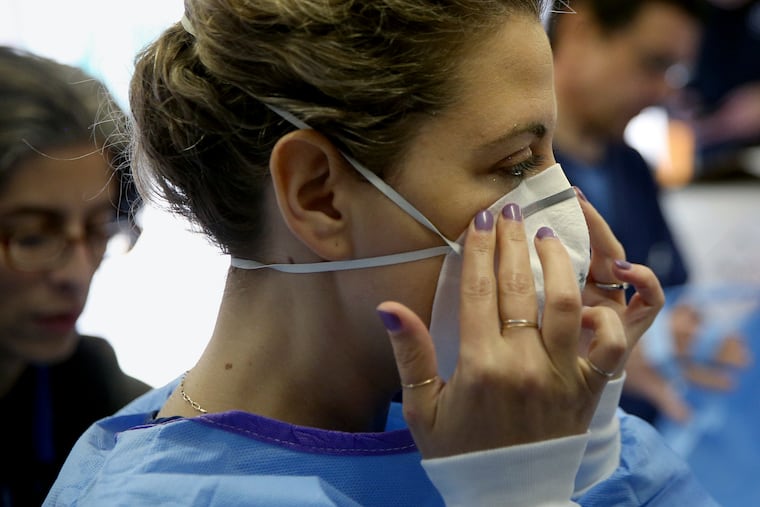
First responders in New Jersey are being advised to buy painters’ masks to protect themselves while treating possible coronavirus patients.
In Pennsylvania, the state Department of Health is reaching out to the mining industry for masks. A hospital in Woodbury, Gloucester County, is asking for mask donations.
Even as the region’s health-care providers are digging in to prepare for the expected wave of coronavirus cases, nurses and doctors are facing no-win decisions due to the lack of personal protective equipment (PPE).
“We don’t have the equipment that we need to properly protect us,” said Maureen May, a nurse at Temple University Hospital and president of the Pennsylvania Association of Staff Nurses and Allied Professionals (PASNAP).
Health-care providers are being encouraged to use N-95 masks, which are dense enough to screen out the coronavirus molecules. But cases are piling up so quickly, May said, that some of the union’s roughly 8,000 members have resorted to reusing the single-use masks. Nurses have been told to store their masks in “a brown paper bag” when not in use to keep the virus contained.
“We shouldn’t be reusing N-95 masks, which is what we are doing, but we don’t have enough so if we get one, we use it over and over again,” she said. "There’s no option.”
It’s a national crisis, said the president of the American Medical Association. “For days, physicians and frontline health-care workers have been sounding the alarm that there is nowhere near enough PPE in the fight against COVID-19 – a shortage that endangers patients and jeopardizes the entire response to this virus,” said AMA president Patrice A. Harris. “Physicians don’t have enough masks; they are wearing a single mask all day, cleaning them at home, and sewing their own protective gear. Confronting COVID-19 requires an all-hands-on-deck approach from federal, state, and local governments, and we urge our leaders to pull every lever at their disposal to ramp up test-kit availability and to equip physicians and the health-care workforce to fight the virus. Anything less is unacceptable at this critical juncture.”
State and local officials acknowledge that they don’t know how much gear is available, much less how much will be needed or where they can get more. President Donald Trump could invoke the federal Defense Production Act to boost production of critical medical supplies, but so far he has not ordered businesses to produce needed supplies including protective gear and ventilators.
“You don’t send a soldier out into a war without a gun,” said Kristen Kucharczuk, a physician with Advocare Main Line Pediatrics, a practice in Narberth and Malvern, “but we are going out there with a stick.”
» READ MORE: Amid coronavirus outbreak, New Jersey’s Lazy Eye Distillery gives out hand sanitizer
As of Friday evening Pennsylvania reported 268 positive cases and one death. New Jersey had 890 cases and 11 deaths.
In Philadelphia, 20 of the city’s 44 confirmed cases as of Thursday were among health-care workers, city officials said. The heavy toll on medical personnel is no surprise, experts said.
“You can do everything in your power not to touch your face, wear gloves,” said David Jaspan, chairman of obstetrics and gynecology at Einstein Medical Center in Philadelphia. “But [the virus] is so prevalent in our environment and your interactions with people who have it, that’s likely the reason” health-care workers are falling to the illness.
The patient with the virus should be wearing a surgical mask and the health-care provider should wear a gown, gloves, eye protection, and a N-95 mask, which are fitted specifically for an individual, Jaspan said. Breathing through them can require some adjustment. It’s in place properly, he said, if a wearer feels a sucking sensation against the face when inhaling.
» READ MORE: A face mask probably won’t protect you from coronavirus. Here’s what can help.
The Pennsylvania Department of Health shipped gloves, N-95 masks, and gowns to 40 counties Thursday, said Nate Wardle, the agency’s spokesperson, though he would not say how many of each were sent.
“It is a continued need,” Wardle said. “Just because we sent some out does not mean we are not going to continue needing more.”
The department is also reaching out to businesses, including the mining industry, Wardle said, to obtain more N-95 masks, or at least similarly protective masks.
“Mining is one of the businesses in Pennsylvania that is considered nonessential, so potentially we could get some,” he said.
The state, like much of the nation, is still figuring out what it has and what it will need.
“I don’t know whether there’s been a request for ventilators," Wardle said. “We are working to try to figure out what we have in Pennsylvania.”
» READ MORE: Coronavirus ‘roller coaster’ will last months, not weeks, experts predict
Protective gear also is essential for health-care workers at the growing number of testing sites.
“We haven’t gotten to the point yet where we don’t have enough protective equipment to do testing,” said Thomas Farley, Philadelphia’s health commissioner. "We hope we won’t get to that point. If we do, we’ll just somehow improvise to work through that problem.”
The health department is also preparing for much higher demand at hospitals, said spokesperson James Garrow. Beds, personal protective equipment, and respirators are all being reviewed citywide, he said, and organizations are requesting donations. The Chamber of Commerce for Greater Philadelphia on Friday night put out a call for supplies including thermometers, sanitary wipes, masks, and gowns.
“We are concerned about the possibility of a surge of patients outstripping our region’s supply and are actively working to see how the region can supplement those supplies,” Garrow said.
The timing and size of the surge, however, are still unclear.
"You look at Italy, you look at Iran, you look at China, it happened very, very rapidly,” said Arvind Venkat, an emergency physician at Allegheny General Hospital in Pittsburgh and president of the Pennsylvania chapter of the American College of Emergency Physicians, with about 1,800 members statewide.
Medical personnel reusing N-95 masks concerns Venkat. If they’re going to be reused, he said, they have to be handled and stored very carefully, and cleaned thoroughly. It’s not an ideal situation, he said, and could endanger physicians and their families.
“Emergency physicians, when they come home, they are disrobing and bathing before they enter any other part of their house,” Venkat said.
» READ MORE: Dealing with mental health and the coronavirus: ‘It’s triggering.’
Small medical practices, meanwhile, have scrounged and innovated.
“Doctors who are allergists, dermatologists, who have to see patients,” Kucharczuk said, “have nothing.”
Kucharczuk, the Main Line pediatrician, has had to improvise solutions, including canceling all but the most necessary appointments. Her practice received mask donations from contractors, a farm in New Jersey, and auto mechanics, enough for each doctor to have one mask for each office throughout the epidemic. She also got face shields from a nearby orthodontist’s office.
“It’s been a very heartwarming outreach from the community,” she said. “People are willing to help."
In Camden, Cooper University Health Care sent a memo to the area’s emergency medical services squads advising them to shop for masks at hardware stores, insulation suppliers, and paint stores.
“Smaller retailers with no online presence may be your best options,” the memo states.
After New Jersey Gov. Phil Murphy ordered nail salons and other nonessential businesses to close by Thursday at 8 p.m, staff at Inspira Health, which runs a 210-bed hospital in Mullica Hill, N.J., jumped on the phone to ask companies if they would be willing to donate — or sell — their masks, said Nick Dalsey Jr., Inspira’s development director.
Masks intended for one-time use degrade over time, becoming less protective, said Michael Menz, a certified industrial hygienist who owns an environmental firm in South Jersey.
» READ MORE: What are the first symptoms of the coronavirus?
Menz said that while he doesn’t have any N95 masks, he does have two respirators with sophisticated filters that he had used for asbestos inspections and other environmental jobs before the crisis curtailed business.
“If there is a doctor or nurse who wants a respirator that can be sanitized, I will drive it to them immediately,” Menz said Friday night.
Some community groups are mobilizing to try to supplement medical providers’ equipment options. On Facebook, the group Sew Face Masks Philadelphia #AbolishCOVID is seeking people to contribute designs and materials as a first step to jump starting a collective effort to make protective masks.
Medical staff will need to ration the equipment they have, Jaspan said, being careful to save the most protective gear for specific tasks. Asking screening questions in person, he said, can be done safely without any protective gear if the medical provider stays six feet away from the patient. If a patient’s symptoms and history suggest coronavirus infection, but the provider isn’t directly treating them, a mask and goggles will suffice. The most protective gear, a gown, gloves, eye protection, and mask, should be reserved only for medical personnel who are in close, direct contact with a patient who could have the illness.
“If we run out of things we’re going to be using handkerchiefs,” Jaspan said, “and that’s just not acceptable in the 21st century.”
Staff writer Laura McCrystal contributed to this article.


